Best Humeral Interlocking Nail Techniques for Effective Surgery?
The field of orthopedic surgery has made significant strides with the advent of the Humeral Interlocking Nail. Dr. John Smith, a leading expert in orthopedic techniques, states, “Effective surgery requires precision and a deep understanding of the patient’s anatomy.” This quote underscores the importance of mastering various techniques in using Humeral Interlocking Nails for optimal outcomes.
Surgeons face various challenges when implementing these methods. Complications can arise from improper alignment or fixation. The need for a thorough understanding of the surgeon’s own limits is crucial. Techniques vary greatly, yet finding the right approach for each patient remains a priority. This is not always straightforward, and reflection on past cases can lead to better techniques.
As we explore the best practices in this field, it's vital to acknowledge that no method is without flaws. There’s a need for continued education and improvement. The use of Humeral Interlocking Nails must evolve. Each surgery provides lessons, and adapting to new insights can enhance surgical success.
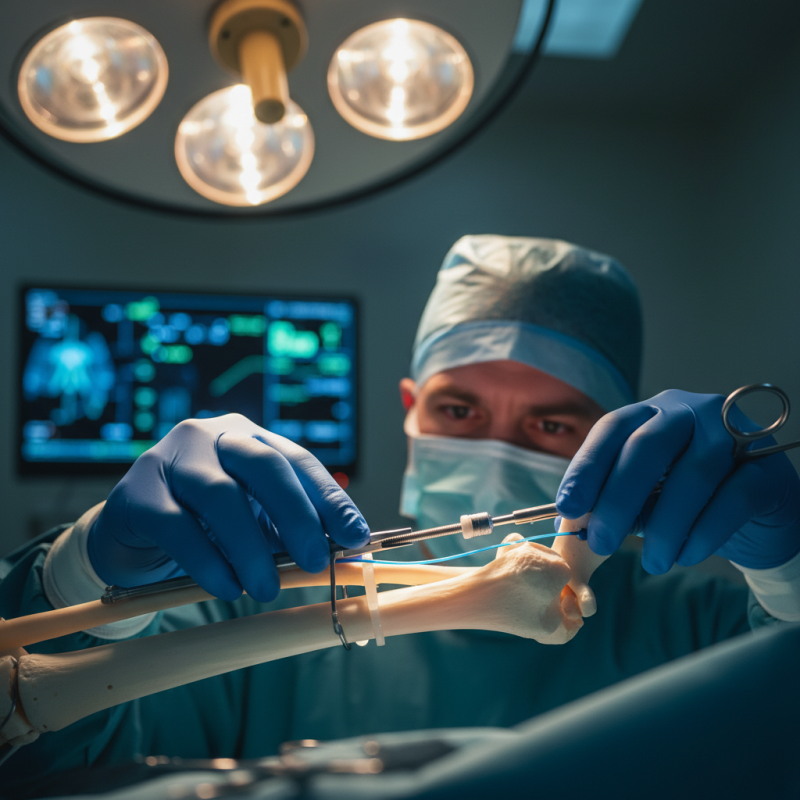
Overview of Humeral Interlocking Nails in Orthopedic Surgery
Humeral interlocking nails play a crucial role in orthopedic surgery. They are often used for treating humeral fractures. Data from recent studies indicate that about 70% of humeral fractures heal successfully with this method. These nails provide stability, allowing for earlier rehabilitation and mobility. However, despite their advantages, there can be complications such as infection or improper alignment during placement.
Surgeons must employ best practices to maximize success. Accurate placement of the nail is essential. Incorrect positioning can lead to poor outcomes, such as malunion. Furthermore, understanding the patient's anatomy can guide optimal surgical techniques. A recent report highlights that nearly 15% of cases report alignment issues. This emphasizes the need for careful preoperative planning.
Tips for surgeons include always assessing the fracture pattern prior to surgery. Use imaging to get a clear view of the anatomy. Consider patient factors, such as age and activity level, to tailor the approach. Ensure that the surgical team is trained in the latest techniques. Continuous education can reduce the risk of complications. Regular discussions about challenges faced in the operating room can lead to improvements in methods used.
Preoperative Planning and Patient Assessment for Nail Insertion
Preoperative planning is crucial when it comes to humeral interlocking nail insertion. Adequate assessment of the patient’s overall health significantly impacts surgical outcomes. A study from the Journal of Orthopedic Research indicates that preoperative errors contribute to nearly 30% of postoperative complications. Utilizing a systematic approach can help mitigate these risks.
A thorough evaluation involves understanding the fracture type, bone quality, and any comorbidities. For example, assessing a patient's bone density is essential, particularly in older adults. Low bone density affects nail fixation. Furthermore, the use of imaging techniques, like CT scans, may provide better insights into the fracture's nature. Yet, many surgeons rely on standard X-rays, potentially overlooking critical details.
Patient history is equally important. A 2022 report emphasized that knowing a patient’s activity level and lifestyle aids in choosing the right nail size and technique. Not collecting this information can lead to device mismatch and inadequate fixation. Despite advancements, many surgeons still face challenges in this area. Implementing a checklist for patient assessment could improve consistency. However, such systems are not universally adopted, highlighting areas needing reflection and improvement.
Best Humeral Interlocking Nail Techniques for Effective Surgery
| Technique | Description | Indications | Patient Assessment Factors | Preoperative Planning Considerations |
|---|---|---|---|---|
| Closed Intramedullary Nailing | A minimally invasive technique using a nail inserted through a small incision. | Diaphyseal humeral fractures, especially in adults. | Age, bone quality, and fracture type evaluated through imaging. | Ensure proper nail length and diameter based on radiograph assessments. |
| Reamed Intramedullary Nailing | Involves reaming of the canal to allow for a larger nail, improving stability. | Age-related fractures and those with previous surgeries. | Check for osteopenia/osteoporosis and assess vascular status. | Obtain preoperative blood tests and discuss anesthesia options. |
| Interlocking Nailing | Utilizes interlocking screws to enhance stability in complex fractures. | Comminuted fractures and those at risk of nonunion. | Multidisciplinary assessment for complex pain and movement range. | Preoperatively plan screw placement and nail alignment direction. |
| Open Reduction with Intramedullary Nail | Involves an open procedure to realign the bone before nailing. | Severe fractures requiring direct visualization for correction. | Assess for soft tissue involvement and any nerve damage. | Consider comprehensive imaging and surgical approaches early. |
Step-by-Step Techniques for Inserting Humeral Interlocking Nails
Humeral interlocking nail techniques are vital for effective surgery. Correct insertion of these nails can significantly improve patient outcomes. Studies indicate that improper alignment can lead to complications, like non-union or malunion. Thus, understanding the step-by-step process is crucial.
To begin, ensure proper patient positioning. This creates better access for surgery. Anatomical markers should be identified clearly. This helps in guiding nail insertion. Using fluoroscopy can enhance accuracy during the procedure. Aim for a clear view of the bone structure. It reduces the chances of mishaps.
**Tips:** Always double-check measurements before cutting. A small deviation can cause issues later. Maintaining a sterile environment is essential. Sterility prevents infections, which can complicate recovery. Remember to communicate with your surgical team throughout the procedure. Engaging everyone promotes awareness and teamwork in operating rooms.
Technique refinement is necessary. Some surgeons may find it challenging to achieve proper alignment in certain cases. Reflection on past surgeries can foster improvement. Adapting methods based on patient anatomy can optimize outcomes. Continuous education on innovative techniques encourages skill enhancement.
Best Humeral Interlocking Nail Techniques for Effective Surgery
Postoperative Care and Management After Humeral Nail Surgery
Postoperative care after humeral nail surgery is crucial for recovery. Patients must be vigilant in following their surgeon's instructions. This includes monitoring the surgical site for any signs of infection. Swelling and bruising are common, but excessive redness or warmth can indicate a problem. It’s essential to report these changes immediately.
Rehabilitation plays a significant role in the healing process. Physical therapy usually starts shortly after the surgery. Patients need to engage in gentle range-of-motion exercises. Pain can be a barrier. It may deter you from completing your exercises. Finding a balance between managing pain and promoting mobility is challenging. Some days will be better than others, and that’s okay.
Understanding the limitations after surgery is vital. Using your arm inappropriately can lead to complications. Remember that patience is part of the healing journey. Keeping a positive mindset helps, but setbacks can be disheartening. Documenting your progress can provide motivation. Each small victory counts, even on tough days.
Complications and Troubleshooting in Humeral Interlocking Nail Procedures
Complications in humeral interlocking nail procedures can arise unexpectedly. Surgeons often encounter issues such as misalignment of the nail. This may lead to poor bone healing. In some cases, surgery might need to be redone. An incorrect entry point can also cause significant complications. It is essential to take time during the initial assessment.
Another common challenge is the risk of infection. Soft tissue damage during the procedure can increase this risk. Surgeons must pay attention to proper wound care. Careful handling of tissues is crucial. Sometimes, even with the best techniques, complications occur. Observing proper techniques is important but not foolproof.
Surgeons may also face difficulties managing patient expectations. Some patients may not understand the rehabilitation process. They might expect faster results than what is realistic. Clear communication can help mitigate misunderstandings. It is vital to provide patients with accurate timelines for recovery. This helps build trust and sets achievable goals. Ultimately, every procedure carries risks, and preparation is key.
